Has your weight loss plateaued? Are you struggling to meet your weight loss goals? Have you struggled to lose weight in spite of doing everything “correctly?” Are you still struggling with those last few pounds?
You’re not alone. Many of my patients, myself included, have found themselves “stuck” in their weight loss progression. There are a number of reasons you may not be loosing weight, but one that I am seeing more and more frequently is “Pseudo-Cushings’s Syndrome.” Pseudo-Cushing’s Syndrome is a physiologic
hypercortisolism (high level of cortisol) that can be caused by a number of problems:
- Physical stress
- Severe bacterial or fungal infection
- Malnutrition or Intense chronic exercise
- Psychological stress – including untreated or under-treated depression, anxiety, post-traumatic stress, or dysthymia (chronic melancholy)
- Alcoholism
The psychiatric literature suggest that up to 80% of people with depressive disorders have increased cortisol secretion (1,2,3). 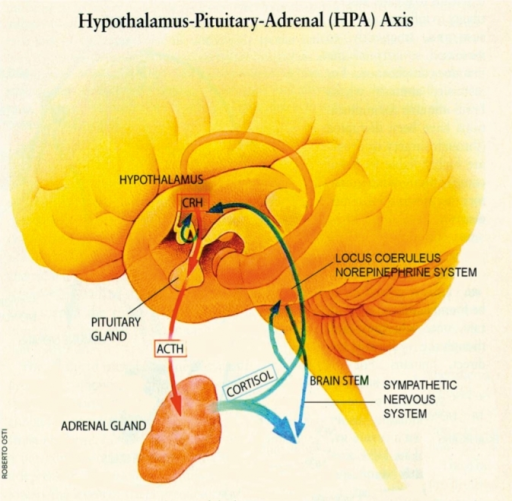 People with significant stressors in their life have been show to have a raised cortisol secretion. Chronic stress induces hyperactivity of the hypothalamic-pituitary-adrenal axis causing an over production of cortisol and normalization of their cortisol levels occurs after resolution of the stressor. This cortisol response is not high enough to lead to a true Cushing’s Syndrome, but effects ones ability to loose weight.
People with significant stressors in their life have been show to have a raised cortisol secretion. Chronic stress induces hyperactivity of the hypothalamic-pituitary-adrenal axis causing an over production of cortisol and normalization of their cortisol levels occurs after resolution of the stressor. This cortisol response is not high enough to lead to a true Cushing’s Syndrome, but effects ones ability to loose weight.
I suspect this is becoming more prevalent due to the high paced, high-stress, always on, plugged in, 24 hour information overload lives we live.
What is cortisol? It is a steroid hormone made naturally in the body by the adrenal cortex (outer portion of the adrenal gland). Cortisol is normally stimulated by a number of daily activities including fasting, awakening from sleep, exercise, and normal stresses upon the body. Cortisol release is highest in the morning, helping to wake us up, and tapers into the afternoon. Cortisol plays a very important role in helping our bodies to regulate the correct type (carbohydrate, fat, or protein) and amount of fuel to meet the bodies physiologic demands that are placed upon it at a given time (4,5,6).
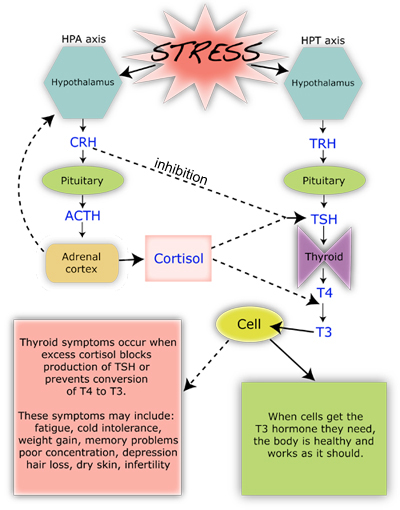 Under a stress response, cortisol turns on gluconeogensis in the liver (the conversion of amino acids into glucose) for fuel. Cortisol, also, shifts the storage of fats into the deeper abdominal tissues and turns on the maturation process of adipocytes (fat cells). In the process, it suppresses the immune system to decrease inflammation during times of stress (7,8,9). In the short run, this is an important process, however, when cortisol production is chronically turned up, it leads to abnormal deposition of fat, increased risk of infection, impotence, abnormal blood sugars, head
Under a stress response, cortisol turns on gluconeogensis in the liver (the conversion of amino acids into glucose) for fuel. Cortisol, also, shifts the storage of fats into the deeper abdominal tissues and turns on the maturation process of adipocytes (fat cells). In the process, it suppresses the immune system to decrease inflammation during times of stress (7,8,9). In the short run, this is an important process, however, when cortisol production is chronically turned up, it leads to abnormal deposition of fat, increased risk of infection, impotence, abnormal blood sugars, head
aches, hypertension and ankle edema, to name a few.
The chronic elevation in cortisol directly stimulates an increase in insulin by increasing the production of glucose in the body, and cortisol blockaids the thyroid axis. Both of these actions halt the ability to loose weight, and drive weight gain.
Cortisol also increases appetite (10). That’s why many people get significant food cravings when they are under stress (“stress eaters”). Cortisol also indirectly affects the other neuro-hormones of the brain including CRH (corticotrophin releasing hormone), leptin, and neuropeptide Y (NPY). High levels of NPY and CRH and reduced levels of leptin have also been shown to stimulate appetite (10-11).
How do you test for Pseudo-Cushing’s Disease?
Testing can be done by your doctor with a simple morning blood test for cortisol. If your cortisol is found to be elevated, it needs to be repeated with an additional 24 hour urine cortisol measurement to confirm the diagnosis. If Cushing’s Syndrome is suspected, some additional blood testing and diagnostic imaging will be necessary.
How do you treat it?
First, the stressor must be identified and removed. Are you getting enough sleep? Is there an underlying infection? Is there untreated anxiety or depression present? Are you over-exercising? These things must be addressed.
Second, underlying depression or anxiety can be treated with counseling, a variety of weight neutral anti-depressant medications or a combination of both. Many of my patients find that meditation, prayer, and journaling are tremendous helps to overcoming much of the anxiety and depression they experience.
Third, adequate sleep is essential. Remove the television, computer, cell phone, iPad or other electronic distraction from the bedroom. Go to bed at the same time and get up at the same time each day. Give yourself time each day away from being plugged in, logged in or on-line.
Fourth, mild intensity (40% of your maximal exertion level) exercise 2-3 days a week was found to lower cortisol; however, moderate intensity (60% of your maximal exertion level) to high intensity (80% of your maximal exertion level) exercise was found to raise it (12). A simple 20 minute walk, 2-3 times per week is very effective.
So, the take home message . . . It’s not the stress that’s killing us, it’s our reaction to it.
References:
- Pfohl B, Sherman B, Schlechte J, Winokur G. Differences in plasma ACTH and cortisol between depressed patients and normal controls. Biol Psychiatry 1985; 20:1055.
- Pfohl B, Sherman B, Schlechte J, Stone R. Pituitary-adrenal axis rhythm disturbances in psychiatric depression. Arch Gen Psychiatry 1985; 42:897.
- Gold PW, Loriaux DL, Roy A, et al. Responses to corticotropin-releasing hormone in the hypercortisolism of depression and Cushing’s disease. Pathophysiologic and diagnostic implications. N Engl J Med 1986; 314:1329.
- Ely, D.L. Organization of cardiovascular and neurohumoral responses to stress: implications for health and disease. Annals of the New York Academy of Sciences (Reprinted from Stress) 771:594-608, 1995.
- McEwen, B.S. The brain as a target of endocrine hormones. In Neuroendocrinology. Krieger and Hughs, Eds.: 33-42. Sinauer Association, Inc., Massachusetts, 1980.
- Vicennati, V., L. Ceroni, L. Gagliardi, et al. Response of the hypothalamic- pituitary-adrenocortical axis to high-protein/fat and high carbohydrate meals in women with different obesity phenotypes. The Journal of Clinical Endocrinology and Metabolism 87(8) 3984-3988, 2002.
- Wallerius, S., R. Rosmond, T. Ljung, et al. Rise in morning saliva cortisol is associated with abdominal obesity in men: a preliminary report. Journal of Endocrinology Investigation 26: 616-619, 2003.
- Epel, E.S., B. McEwen, T. Seeman, et al. Stress and body shape: stress-induced cortisol secretion is consistently greater among women with central fat.
Psychosomatic Medicine 62:623-632, 2000. - Tomlinson, J.W. & P.M. Stewart. The functional consequences of 11_- hydroxysteroid dehydrogenase expression in adipose tissue. Hormone and Metabolism Research 34: 746-751, 2002.
- Epel, E., R. Lapidus, B. McEwen, et al. Stress may add bite to appetite in women: a laboratory study of stress-induced cortisol and eating behavior.Psychoneuroendocrinology 26: 37-49, 2001.
- Cavagnini, F., M. Croci, P. Putignano, et al. Glucocorticoids and neuroendocrine function. International Journal of Obesity 24: S77-S79, 2000.
- Hill EE, Zack E, Battaglini C, Viru M, Vuru A, Hackney AC. Exercise and circulating cortisol levels: the intensity threshold effect. J Endocrinol Invest. 2008. Jul;31(7):587-91.
