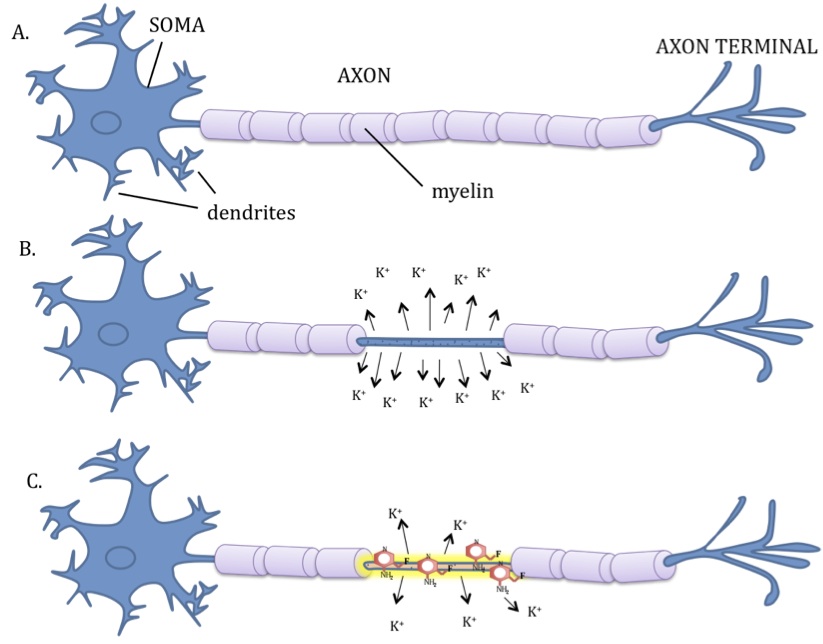
Multiple Sclerosis (MS) is a neurological disease caused by demyelination or breakdown of the myelin coating around the nerve cells (1). This is referred to as a neurodegeneration where the physical structure of the nerve is compromised, much like the coating around an electrical wire being chipped or stripped away. Common symptoms of MS are sensory symptoms in the extremities or face, unilateral visual loss, acute or subacute motor weakness of the muslces, diplopia (double vision), gait disturbance and balance problems, Lhermitte sign (electric shock-like sensations that run down the back and/or limbs upon flexion of the neck), vertigo, bladder problems, loss of control of a limb, and pain.

Initially, and for many years, the degeneration seen in multiple sclerosis (MS) was thought to occur because of an acute inflammatory attack on the cells by dis-regulated immune cells crossing the blood brain barrier. However, treatments focused on modulating the inflammatory attack seem to have no effect on the degeneration and demyelination. Thus, the actual definitive cause of this demyelination and neuro-degeneration has eluded us since 1868, when Jean-Martin Charcot first described it.
Recent studies point to evidence that this demyelation may be due to degeneration or breakdown of the nerve cell’s ability to use glucose as a primary fuel (2, 3). It is now theorized that MS may be due to a combination of degeneration and localized inflammation related to poor glucose uptake causing the demyelination which is seen in a number of MS cases (4, 5, 6).
With this dual concept in mind, ketogenic diets have demonstrated some promising results when used with neurological diseases including MS. Ketogenic diets have been used in the treatment of epilepsy since 500 B.C. and in the treatment of obesity since 1860. It is now becoming apparent that ketogenic diets may play a very significant role in the treatment of neurological disease because of two-fold effects that arise when ketones become the primary fuel for the body.
First, when a person becomes keto-adapted and ketones are used as the primary fuel, instead of glucose, the body up-regulates mitochondria to use the ketones for fuel. As the ketone level rises, the need for glucose diminishes. This provides the nerve cell an alternative fuel source if glucose metabolism is impaired. It also decreases the need and production of insulin, a known hormone heavily involved in stimulating inflammation and inflammatory responses.
The second effect of a ketogenic diet is this favorable effect on inflammation. It has been demonstrated that a ketogenic diet decreases reactive oxygen species, increased production of superoxide dismutase and catalayse, all of which notably decrease the inflammatory effects of oxidative stress (9,10, 11). A ketogenic diet also is well known to raise glutithione levels, another anti-oxidant that decreases inflammation and oxidative stress (12-16). This same anti-inflammatory and keto-adaptation effect can be obtained from intermittent fasting.
To date, studies in patients with neurologic diseases like MS, Alzheimer’s disease using ketogenic diets have had positive results in memory, cognition and diminished inflammation with evidence of halting or reversing the chronic demyelination (17,18, 19). Still somewhat theoretical, the evidence points to effective dietary treatment and prevention for multiple sclerosis and other degenerative neurological diseases like Alzheimer’s Disease.
References:
- J. M. Pearce, “Historical descriptions of multiple sclerosis,” European Neurology, vol. 1, no. 1, pp. 49–53, 2005.
- C.-A. Castellano, S. Nugent, N. Paquet et al., “Lower brain 18F-fluorodeoxyglucose uptake but normal 11C-acetoacetate metabolism in mild Alzheimer’s disease dementia,” Journal of Alzheimer’s Disease, vol. 43, no. 4, pp. 1343–1353, 2014.
- S. Nugent, S. Tremblay, K. W. Chen et al., “Brain glucose and acetoacetate metabolism: a comparison of young and older adults,” Neurobiology of Aging, vol. 35, no. 6, pp. 1386–1395, 2014.
- H. Lassmann, W. Brück, and C. F. Lucchinetti, “The immunopathology of multiple sclerosis: an overview,” Brain Pathology, vol. 17, no. 2, pp. 210–218, 2007.
- C. Confavreux and S. Vukusic, “Natural history of multiple sclerosis: a unifying concept,” Brain, vol. 129, no. 3, pp. 606–616, 2006.
- P. K. Stys, G. W. Zamponi, J. van Minnen, and J. J. G. Geurts, “Will the real multiple sclerosis please stand up?” Nature Reviews Neuroscience, vol. 13, no. 7, pp. 507–514, 2012.
- P. G. Nijland, I. Michailidou, M. E. Witte et al., “Cellular distribution of glucose and monocarboxylate transporters in human brain white matter and multiple sclerosis lesions,” Glia, vol. 62, no. 7, pp. 1125–1141, 2014.
- L. C. Costantini, L. J. Barr, J. L. Vogel, and S. T. Henderson, “Hypometabolism as a therapeutic target in Alzheimer’s disease,” BMC Neuroscience, vol. 9, supplement 2, article S16, 2008.
- P. G. Sullivan, J. E. Springer, E. D. Hall, and S. W. Scheff, “Mitochondrial uncoupling as a therapeutic target following neuronal injury,” Journal of Bioenergetics and Biomembranes, vol. 36, no. 4, pp. 353–356, 2004.
- P. G. Sullivan, N. A. Rippy, K. Dorenbos, R. C. Concepcion, A. K. Agarwal, and J. M. Rho, “The ketogenic diet increases mitochondrial uncoupling protein levels and activity,” Annals of Neurology, vol. 55, no. 4, pp. 576–580, 2004.
- T. Shimazu, M. D. Hirschey, J. Newman et al., “Suppression of oxidative stress by β-hydroxybutyrate, an endogenous histone deacetylase inhibitor,” Science, vol. 339, no. 6116, pp. 211–214, 2013.
- S. G. Jarrett, J. B. Milder, L.-P. Liang, and M. Patel, “The ketogenic diet increases mitochondrial glutathione levels,” Journal of Neurochemistry, vol. 106, no. 3, pp. 1044–1051, 2008.
- J. B. Milder, L.-P. Liang, and M. Patel, “Acute oxidative stress and systemic Nrf2 activation by the ketogenic diet,” Neurobiology of Disease, vol. 40, no. 1, pp. 238–244, 2010.
- N. Dupuis, N. Curatolo, J. F. Benoist, and S. Auvin, “Ketogenic diet exhibits anti-inflammatory properties,” Epilepsia, vol. 56, no. 7, pp. e95–e98, 2015.
- D. Y. Kim, J. Hao, R. Liu, G. Turner, F.-D. Shi, and J. M. Rho, “Inflammation-mediated memory dysfunction and effects of a ketogenic diet in a murine model of multiple sclerosis,” PLoS ONE, vol. 7, no. 5, Article ID e35476, 2012.
- Y.-H. Youm, K. Y. Nguyen, R. W. Grant et al., “The ketone metabolite β-hydroxybutyrate blocks NLRP3 inflammasome—mediated inflammatory disease,” Nature Medicine, vol. 21, no. 3, pp. 263–269, 2015.
- A. Ramm-Pettersen, K. O. Nakken, I. M. Skogseid et al., “Good outcome in patients with early dietary treatment of GLUT-1 deficiency syndrome: results from a retrospective Norwegian study,”Developmental Medicine and Child Neurology, vol. 55, no. 5, pp. 440–447, 2013.
- Y. Ito, H. Oguni, S. Ito, M. Oguni, and M. Osawa, “A modified Atkins diet is promising as a treatment for glucose transporter type 1 deficiency syndrome,” Developmental Medicine and Child Neurology, vol. 53, no. 7, pp. 658–663, 2011.
- M. Storoni and GT Plant, “The Therapeutic Potential of the Ketogenic Diet in Treating Progressive Multiple Sclerosis,” Multiple Sclerosis International, vol. 2015, Article ID 681289, 9 pages, 2015.

